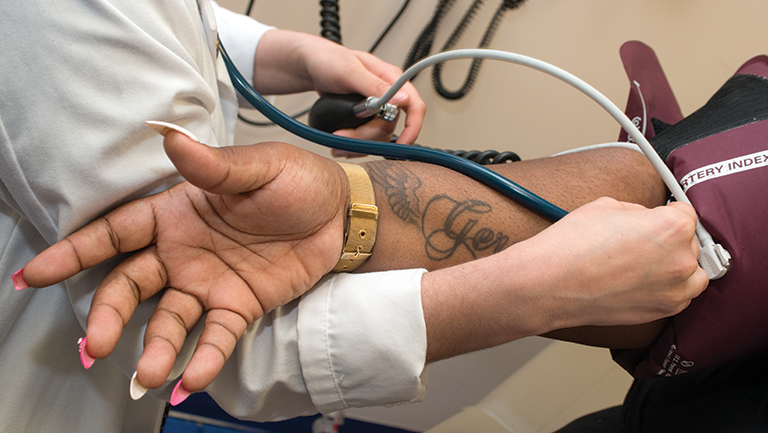
Title:Cura Communitas
Building Health Equity in D.C.
Above: Medical students have cared for thousands of patients since HOYA Clinic opened its doors in 2007.
On a rainy Wednesday night inside the D.C. General Family Homeless Shelter, a woman waits in an examining room of the free clinic run by Georgetown medical students and faculty. Her toddler plays with a few available toys in the area. An African American D.C. resident in her 20s, she recently moved into the shelter with her two children to escape domestic abuse. She has health insurance, but no home, child care, transportation, or primary care provider. And her health is faltering.
“God knows the struggles I’ve seen,” she says. “I’ve been down, depressed, gained weight, lost weight, everything, but hopefully, I’ll be safe here.” Until his court date, her abuser is still on the street. The shelter’s round-the-clock security team provides her only protection—and HOYA Clinic, her only health care.
“I’ve had two doctors here and both were great,” she says. “I only wish it was open every day, not just Tuesday and Wednesday. Sometimes it’s hard to wait, but I know they’ll be here for me.”
Disparity by the numbers
This young mother is one of hundreds of patients seen each year at the HOYA Clinic, which in turn is one of several Georgetown programs seeking to make a dent in a massive local and national problem: racial, ethnic, and socioeconomic disparities in health care. Statistics show that health outcomes and access to care are distinctly and dramatically worse among the District’s poor and ethnic or racial minorities when compared with other groups. Even when the incidence of disease is comparable between racial groups, morbidity tends to be higher for blacks. Indeed, the nation’s capital and surrounding counties are home to some of the most significant health disparities in the United States. For example:
- White males in the District can expect to live 15 years longer than black males. White females can expect to live 9 years longer than black females.
- The incidence of breast cancer is more prevalent among white women than black women, yet black women are 1.5 times more likely to die from the disease.
- Compared to whites, blacks are twice as likely to die from heart disease and twice as likely to die from a stroke.
These inequities are the focus of a recent report prepared by the Georgetown School of Nursing & Health Studies (NHS), led by Christopher J. King, PhD, director of the master’s program in Health Systems Administration. Commissioned by Maurice Jackson, associate professor of history and African American studies and former chair of the D.C. Commission on African American Affairs, the report’s action-oriented aim is in the title: “The Health of the African American Community in the District of Columbia: Disparities and Recommendations.”
The report’s foundational principle is that access to clinical care represents a small fraction of a person’s total health status. The model pegs the impact of a patient receiving treatment by a health care provider at only 20 percent. Forty percent is caused by social and economic factors, such as income and education. Thirty percent is determined by behaviors such as diet and exercise. One’s physical environment, such as air and water quality, is 10 percent.
“Racial differences in health may be caused by structural or institutionalized injustices in social, economic, political, and environmental systems,” the report states. D.C. has one of the highest insured rates in the nation, with more than 90 percent of black residents currently insured and more than 98 percent of black children covered by insurance. But even with high rates of insurance coverage, poor health outcomes remain.
A moral and institutional imperative
The NHS report aligns with a broader, university-wide effort to address many of the institutional underpinnings that impact racial disparities in American society. As President John J. DeGioia noted in 2016, “An institution with our distinct set of characteristics must engage the continuing challenges that flow from the tragic history of slavery and segregation of our nation. Persistent differences in educational outcomes, health disparities, economic participation—the increasing inequalities across our nation—all require a sustained and enduring commitment that only the Academy can provide.”
Recognizing the complexity of health disparities’ causes and impacts, Georgetown has marshalled resources across campuses to do what no one program could do individually.
At Georgetown University Medical Center (GUMC), Lucile Adams-Campbell, PhD, and Phyllis Magrab, PhD, lead a university-wide effort to address health disparities in Washington, D.C. and beyond. Adams-Campbell is an epidemiologist and expert on health disparities who serves as the associate director of minority health and disparities at Georgetown Lombardi Comprehensive Cancer Center, as well as the associate dean of community health and outreach. Magrab is a pediatric psychologist who has championed underserved populations and directs the Center for Child and Human Development. Through research, education, and outreach, they work with faculty across the university to identify, understand, and reduce disparities in health and health care in communities around the world, and in Washington, D.C.
Within the Medical Center, the breadth of health-disparities work at the School of Nursing & Health Studies alone offers an example of the kinds of programs being undertaken to address the issue. Along with the recent report on D.C. health disparities, NHS is housing the CDC-funded Mid-Atlantic Center for Children’s Health and the Environment, leading a campuswide Population Health Initiative, partnering with Mary’s Center and Briya Public Charter School on a medical assistant training program, offering a new three-credit undergraduate course on health equity, and developing community health needs assessments as a part of class.
And that’s only the beginning.
“I know a lawyer…”
In November, as part of the focus on health disparities, Georgetown established D.C.’s first university-based medical-legal partnership (MLP): the Georgetown University Health Justice Alliance, a collaboration between Georgetown University Medical Center and Georgetown University Law Center.
Nationwide, increasing awareness of the impact of legal problems on health outcomes has generated a growing number of alignments between the medical and law professions. A medical-legal partnership enables lawyers to coordinate directly with health care providers to treat patients holistically, helping to prevent legal and health crises. Found now in 41 states and the District, MLPs offer legal services as part of patient care.
“When you’re talking about the social determinants of health, there is often a legal dimension, an unmet legal need,” says Vicki Girard (L’87), professor of legal research and writing at the Law Center and co-director of the Health Justice Alliance. “People don’t realize the rights they have. A woman who is pregnant may have a cause of action against her boss for cutting her hours down as she approaches maternity leave, or parents with a child who repeatedly misses school for chemotherapy treatments may not know that they have a right to educational support to help their child keep up academically.”
Doctors contribute to the success of an MLP by serving as front-line screeners for legal needs, making patient referrals, and collaborating with attorneys in advocacy efforts. An MLP can mobilize legal resources to address a wide range of social determinants of health, including problems associated with public benefits access, immigration status, employment, education, family law, end-of-life planning, domestic violence, and physical or mental disability.
“We will train health care professionals to recognize issues that may benefit from legal intervention,” says Girard. Through the MLP, the Law Center will assign students to provide direct legal services. The partnership offers lawyers a way to help people with things that the doctor cannot remediate alone. “Patients’ trusting relationship with their health care providers means that physicians are uniquely positioned to connect patients with the legal help they may need,” Girard explains. “If the lawyers can train health care providers on the front line, together we can prevent more severe problems going forward.”
Eileen Moore, MD, medical director of the partnership, adds that it will enable patients to receive more holistic care. “It is my hope and my expectation that the alliance will empower providers to delve deeper into the critical elements of each patient’s history—environment, nutrition, exercise, and personal habits,” she says.
“I cannot tell you how many times I have recommended that patients take time off work to address their medical needs, but many won’t do it for fear of being fired,” Moore says. “I can’t stress enough how wonderful it will be to be able to provide pro bono legal assistance to these patients.”
The design of the Health Justice Alliance makes student leadership a cornerstone, taking advantage of both the law clinic model and the student-driven health clinic. Law clinic students will train medical students and health care workers across the medical spectrum to recognize issues that need legal intervention. Health care providers will then make referrals for direct legal services.
The Health Justice Alliance is also looking at disparities in Washington, D.C. in the area of oral health. The District’s population has one of the highest rates of oral care coverage for Medicaid-enrolled children with special health care needs in the nation, yet simultaneously the lowest utilization for that group. Georgetown’s Health Justice Alliance is working to determine what barriers to oral care might exist for these children. Likely among them are low reimbursement rates for Medicaid patients and added provider education and training, which together impact the ability of a dentist to spend the extra time required for special needs care. Transportation issues, time off from work for parents to keep appointments, and lack of information may also make dental care a low priority for lowincome families.
The alliance will undertake a survey of dental providers to identify and address barriers to effective oral health care. Students will explore best practices, such as the New Mexico Special Needs Dental Procedure Code, which offers providers a monetary incentive for treating patients with special needs. Adams-Campbell cites the case of a 12-year-old African- American boy in Prince Georges County, Maryland who came home from school one day complaining about a headache caused by an infected tooth. Less than two months later, the child died from complications related to the infection.
“No one should die because of lack of access to or knowledge about oral health and dental care,” Adams-Campbell says.
Lessons learned from the homeless
To help address such issues around access to care, Georgetown students meet many underserved D.C. patients where they are: at the homeless shelter.
On a site that also houses the city jail, the morgue, a methadone center, and an alcohol rehabilitation unit, the D.C. General Family Homeless Shelter can feel like a foreboding place. Decades of Georgetown medical students had rotations at the former hospital, the city’s first and only public one, which closed in 2001. The building was converted to a temporary homeless shelter shortly thereafter—ostensibly for one year only. Plans to close it permanently have been hampered by the complexities of finding replacement spaces. It now provides shelter for more than 200 families.

At HOYA Clinic, students gather with medical director, Eileen Moore, MD, to review cases.
This year, the HOYA Clinic will mark a decade of providing medical student-driven and faculty-supervised care for the homeless community at D.C. General, in partnership with MedStar Georgetown University Hospital. “The clinic began through the efforts of a dedicated group of Georgetown medical students who raised money to create the original clinic in D.C. Village—a family shelter closed one year later by the city,” recalls Stephen Ray Mitchell, MD, dean for medical education. “The students followed city plans with presence, advocacy, and dedication until the city agreed to help rebuild the clinic inside the old D.C. General.”
Now operating on the fourth floor of the shelter, HOYA Clinic offers free walk-in care to the greater community of underserved and underinsured D.C. residents. The facility is a federally inspected, student-driven clinic with electronic health records, a fully stocked, free primary-care pharmacy, an innovative program of referral, and health education.
The clinic has served thousands since its founding 10 years ago and, at the same time, has provided hundreds of Georgetown medical students with unparalleled clinical experience. Students engage in patient-centered care, collaborating with patients to understand and address their individual health needs. On any given evening, the clinic is staffed with first-, second-, and third-year students, as well as a resident and attending physician, with the more advanced students assisting in teaching. The experience is so popular that a first- or secondyear student might only have the opportunity to work at HOYA Clinic one or two times per year.
George Koch (M’18), a third-year student who has logged multiple hours at the clinic, says that one key to the program is that everyone learns from each other. “It’s so team-oriented and service-oriented. You’re not just helping the patients; you’re serving the other students. You really feel part of a community.”
On a slow night, the students go down to the shelter and talk to the residents. “We try to find out what their needs might be and how we can help,” Koch says. The HOYA Clinic puts a special emphasis on pediatric care, he says. “There’s a real toxic threat that goes with that living situation and children are the most vulnerable. Sometimes the adults don’t want to talk to us, but we reach them through the kids, who always want to talk. The kids constantly surprise me with how tough they can be. They just want to be kids.”
On a recent evening, a small team of students and a resident gather with the clinic’s medical director, Eileen Moore, MD, to review cases. As two first-year students conduct patient presentations for their first time, Moore nods. They report the patient’s symptoms—pain, nausea—and she asks more questions, which the students answer with care.
“I see evidence of some good coaching here,” she tells the group.
Each night, the attending physician holds a “Teaching Moment” with one case discussed in detail. This night’s patient, an older man with asthma, has been coming to the clinic for years. He is here primarily because he has run out of medication and cannot refill his prescription without a fixed address.
“Did anything we saw tonight surprise or disturb you?” Moore prods as the students take turns responding. “How do we know if it’s asthma and not chronic bronchitis? What can we learn about wheezing? How many kinds of wheezing are there? What do we know if there is no wheezing?”
Another patient has come to the clinic tonight for her first time. When two more students come in to ask her follow-up questions, she answers patiently, grateful for the free care and the attentive clinicians who are obviously learning. She says, “I like that they have the students shadowing. It’s a cool way for them to get hands-on experience.”
The gratitude goes both ways.
Dean Mitchell, a pediatrician and internist, also works regularly at the clinic. The patient-centered care provided there is deeply valued, he says, and it also has an effect beyond the D.C. community. “Our students have had ongoing positive impact on the marginalized of our city, but those patients have helped to form incredible, caring doctors for the rest of the world.”
“As I look at our graduates over the last decade, I think back to those students with whom I personally spent time at HOYA clinic,” Mitchell adds. “I can count a chief medicine resident at Duke, a surgery chief at University of Southern California, and especially the energetic pediatrician who pushed to get HOYA reopened when the city closed it, now running a primary care clinic in the Midwest.”
Mapping the path for patient care
In addition to the HOYA Clinic, for more than a decade Georgetown has offered community-based breast cancer screening to patients with and without insurance in underserved areas of the District. The Georgetown Lombardi Capital Breast Care Center is expanding its range of services and life-saving interventions this year. Capitalizing on its clinical partnership with MedStar Health, CBCC will make it easier for women to find breast cancer screening and treatment options in numerous convenient locations around the Washington area.
The center will continue helping patients get screenings even if they do not have insurance, but will also provide patient transportation, and plans to offer patient navigation to help with appointment scheduling and follow-up care. The services will reach an expanding population for the center, which will offer colorectal, lung, and prostate cancer screening later this year. “We remain committed to reducing the burden of cancer in underserved communities,” says Adams-Campbell. “We’re excited about the potential offered by expanding our services.”
Inspired in part by the success of CBCC, Georgetown’s Lombardi Comprehensive Cancer Center anticipates launching its own Health Disparities Navigation Project. The initiative would create one of the most comprehensive health care navigation programs in the region—one that not only connects patients to treatment, but also educates communities about cancer prevention, screens high-risk populations, and helps patients overcome personal barriers to obtaining care, such as language barriers or lack of transportation or child care. The program could significantly reduce cancer outcome disparities that currently exist in the greater D.C. area and serve as a model for intervention in cities across the country.
Uncertainty ahead
With health policy in flux under the new presidential administration, the future availability of resources to meet the health needs of D.C.’s underserved is unclear. A Senate bill introduced in January, for example, would ban federal funding for tracking “community racial disparities or disparities in access to affordable housing,” raising concern among health care advocates about the ongoing ability to quantify and address health disparities.
How is Georgetown contending with this uncertainty?
“Whatever happens, we need to look at it from our Jesuit perspective—it is a social justice issue,” says Magrab. “How do we step up as a faith-based institution? What would success look like? All people deserve health care—primary care and chronic condition care. Every other westernized country has figured it out. Shame on us if we don’t find a way to do it.”

Mindfulness meditation is an increasingly popular treatment for anxiety, but testing its effectiveness in a convincing way has been difficult.
A synthesized steroid mirroring one naturally made by the dogfish shark prevents the buildup of a lethal protein implicated in some neurodegenerative diseases.
A recent study of New York State’s expansion of access to care reveals unexpected results.